Is eating and talking an uncomfortable experience for you? Does smiling not come easy anymore? Does being in public lead to awkward situations which you feel may negatively impact your social life, daily lifestyle, and self-confidence?
Experts have called dental implants the Cadillac or Ferrari of dental restoration. It may sound flattering, but it is accurate. It is inarguably the best option available to replace a missing tooth. Even more so because of its versatility.
Dental implant specialists can use an implant as a solid foundation to replace a tooth, multiple teeth, or an entire row of teeth.
Learn More about Dental Implants
Tooth Replacement
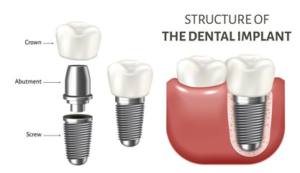
A Dental Implant for tooth replacement consists of three parts:
- A titanium dental implant, serving as the root;
- Abutment (also appropriately called a connector)
- Crown, the visible white part serving as the tooth and modeled to look like your other natural teeth
When the procedure is complete a tooth implant looks like, has the same structure as, and functions like a natural tooth.
- Implants can last a lifetime, have the highest success rates, and serve as a long-term, cost-effective tooth restoration. Alternatives such as crowns, bridges, and dentures are usually only good for 5-10 years.
- Implants are good news for other structures in your mouth. As they:
- help stimulate and preserve the jawbone that’d otherwise deteriorate,
- prevent gums from receding, and
- provide essential protection to neighboring teeth (and do not compromise the health of adjacent teeth)
- Implants offer excellent stability, strength, and functioning. You’d be able to eat your favorite foods and savor the full taste of food. You’d not have to cope with slips, slides, shifts, or clicks and the inevitable “repositioning” you have to do; which may be embarrassing, uncomfortable, make you mumble or slur your words, make chewing difficult, or make your smile look unnatural
- Implants are easy to care for. You can brush and floss a tooth implant as you would your other teeth. All that is required to ensure maximum durability is to care for your gums and teeth regularly and keep your dental appointments (as you should even with natural, healthy teeth).
Alternatives, on the other hand, don’t help much in preserving the health of other mouth structures. Some other options such as a tooth-supported fixed bridge, require damaging other healthy teeth. With dental implants you can laugh, smile, and converse more as you would with healthy, fully functional natural teeth. This makes you feel better about yourself and join in on the fun effortlessly. Your teeth (or lack thereof) no longer dictates how you lead your life, you do!
Addy's Dental Implant Experience
Dental Implant Process
Consultation
This is when you have a sit-down to go over your interest in a dental Implant. It entails everything from finding out if you are a candidate for a dental Implant restoration to knowing what the procedure would cost you.
This examination may include:
- visual inspection
- use of photographs
- x-ray imaging
- [3D] CT (computed tomography or CAT) scans—Panoramic View and/or Cone Beam CT scans
Our dental professionals will conduct these tests to evaluate your gum health, quantity and density of your jawbone, and determine the appropriate location to place the implant(s).
The dental specialist would use information gleaned from the examination to prepare a detailed treatment plan. The specialist would discuss details of the plan and other important information with you. Each treatment plan is specifically tailored to your mouth and needs. We will be completely transparent ensuring you understand all options available to you.
Surgery
Options for your surgery include, local anesthesia (you’re awake, but the surgical area is numbed) or IV Sedation (where you sleep comfortably and remember nothing). Next the site will be prepped for the implant. The implant post will be screwed into the bone and then sutured. Osseointegration will begin to occur over the next few months until you are ready to receive your crown. On average, a properly placed and well-maintained dental Implant prosthetic would last for more than 50 years.
Recovery
The following are some of the common post op instructions:
- Take ibuprofen, other prescribed pain medication, and/or antibiotics
- Use an ice pack or package of frozen vegetable for 10 minutes on and 10 minutes off to reduce swelling
- Rise gently with warm salt water for a few days after the procedure to soothe the gum tissue and for added relief
Additionally, for about 7 days after the procedure, you would have to stick to diets comprising only soft foods and not eating on the site of the surgery.
Care and Maintenance
Tooth Implant
Care for it like you would a natural tooth.
- Regular brushing (at least twice a day) and flossing (at least once a day)
- Rinsing with antibacterial mouthwash or salt water.
Always avoid smoking as it is attributed to higher failure rates.
Healing time
On average, a dental Implant restoration would take three to six months to complete. If you need to have additional procedures done, such as bone grafting or treatment for periodontal disease, the duration could stretch out to nine months.

