Watch this FIRST before proceeding with Gum Disease Treatment
Periodontal Disease Options
Have you been told you have gum disease, also known as periodontal disease, and you were not sure about the treatment options they recommended? Ever wonder what is gum disease and how did this happen when you don’t even feel any pain? Well, I’m here to explain this to you. If you want to watch the video, then feel free to as it’s the same information as in this post.
Gum Disease | McKinney Texas | Plano Texas | Grapevine Texas
So, what is gum disease? Gum disease is a situation where bacteria in the form of plaque or tartar, gets underneath your gums and therefore releases toxins that cause your gums to be inflamed, and eventually also causes you to lose the bone surrounding your teeth. The sad thing about this is that gum disease is actually the reason that most adults actually lose their teeth. Most people usually think it’s cavities, but it’s actually gum disease. In addition, undiagnosed gum disease is the #1 reason for lawsuits in dentistry.
How Do We Diagnose Gum Disease?
The majority of times patients don’t even know they have gum disease. They say, “well doc, I don’t feel any pain.” Well, there are so many other situations in life that we might not have pain. You could have high blood pressure. You can have high cholesterol. You could have many different situations in your life like cancer where you can have a situation where you don’t feel anything till it’s too late. We don’t typically use pain as a precursor to telling us whether we have a disease or not. So how would we diagnose gum disease? Well, we do two major things.
- We examine your x-rays and
- We also measure your gums.
Examining x-rays
So, taking a look at your x-rays, I know a lot of times you go to the dentist’s office and you don’t even really know what you’re looking at. I don’t blame you because if I was to look at an MRI if I went to the hospital, I wouldn’t know exactly what I’m looking at either.
Healthy Bone
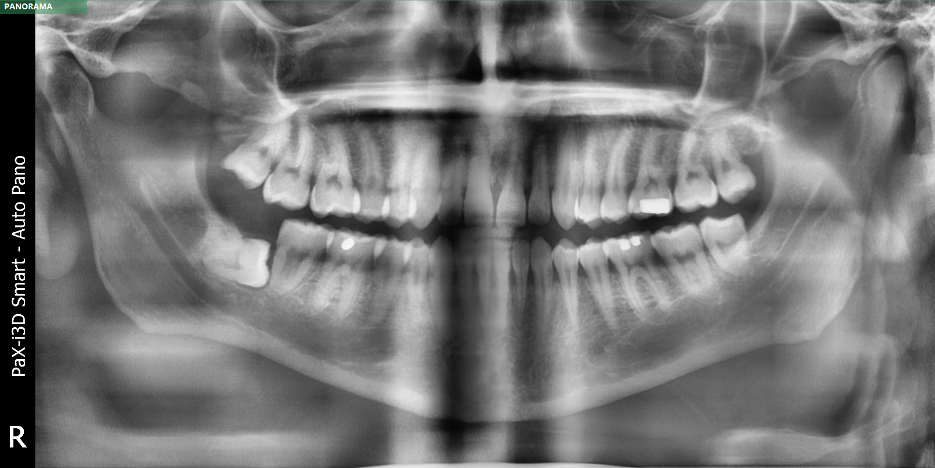
This is what healthy bone and gum look like. The bone is right around what we call the crown of the tooth. The crown is the visible part of the tooth that we see in your mouth. But on this x-ray, we can see that the bone is pretty close to the crowns of your teeth.
Mild Periodontal Disease
If you have mild periodontal disease, it typically looks something like the previous picture above. You might see a little bit of bone loss going on. I know to the untrained eye it’s going to be a little bit harder for patients to really see. But usually, you see a little bit of bone loss compared to this previous x-ray I showed you where this patient had no bone loss.
Moderate Periodontal Disease
Moderate periodontal disease on x-rays shows up with a bit more bone loss. You typically see approx. 3-4 mm of bone loss. The red arrows depict areas of approx. 3-4 mm of bone loss
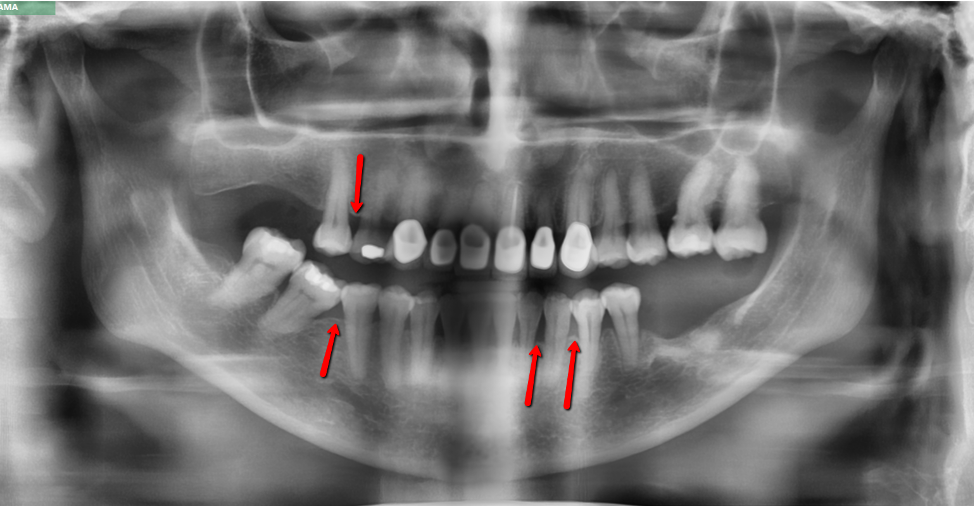
Severe Periodontal Disease
With severe periodontal disease, you typically see about greater than 4mm of bone loss. In this case, this back molar, you see this area of black. That’s really what we’re looking for because when you lose bone, the areas next to the root surfaces become darker. So why do we see darker areas? Well, when the bone is diseased due to the periodontal disease, then what happens is the bone is lost and when the bone is lost, it turns from that nice white, dense-looking bone to a darker shade of gray over here. And that’s what’s indicative of bone loss. So in this X-Ray, this patient has isolated areas of severe bone loss. By the way, I did not place that implant on that patient. I don’t know who did, but this is a terrible implant.
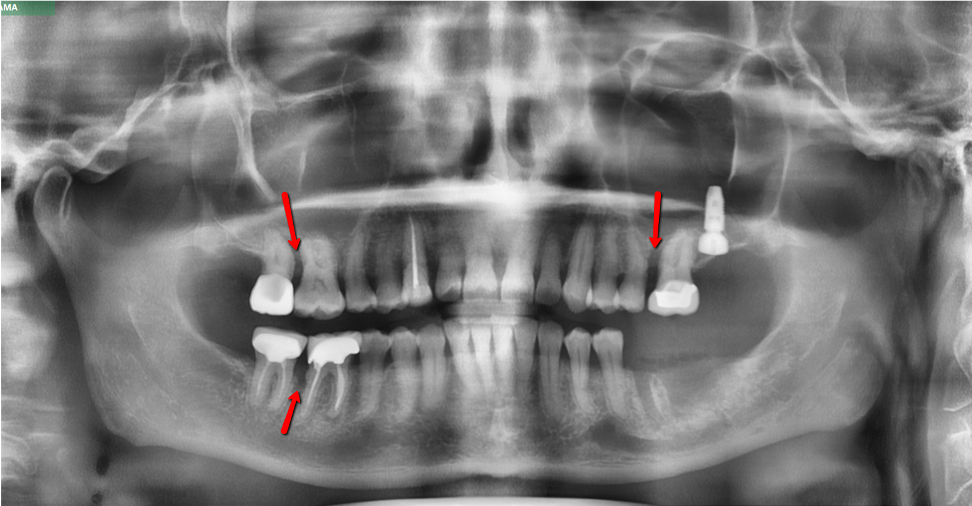
And this is another example of severe bone loss. We can see where the necks of the teeth are and where the bone is. You see these areas of darkness around the roots. And that’s what’s very indicative telling us that this patient has a very severe case, even what we call periodontal abscesses.
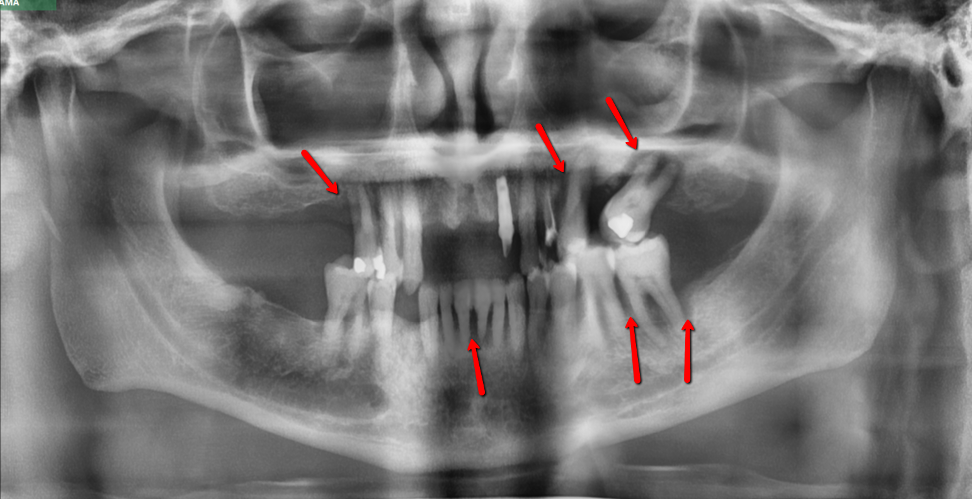
Here’s another example. This patient came to me for a consult regarding implants and unfortunately, somebody placed an implant on him when he had active periodontal disease and therefore is about to lose this implant. But you can see on this x-ray that this patient has a severe bone loss. You could see that the bone is nowhere near the crown of the tooth. And so, this patient has severe periodontal disease and that’s what you would be looking for in these cases.
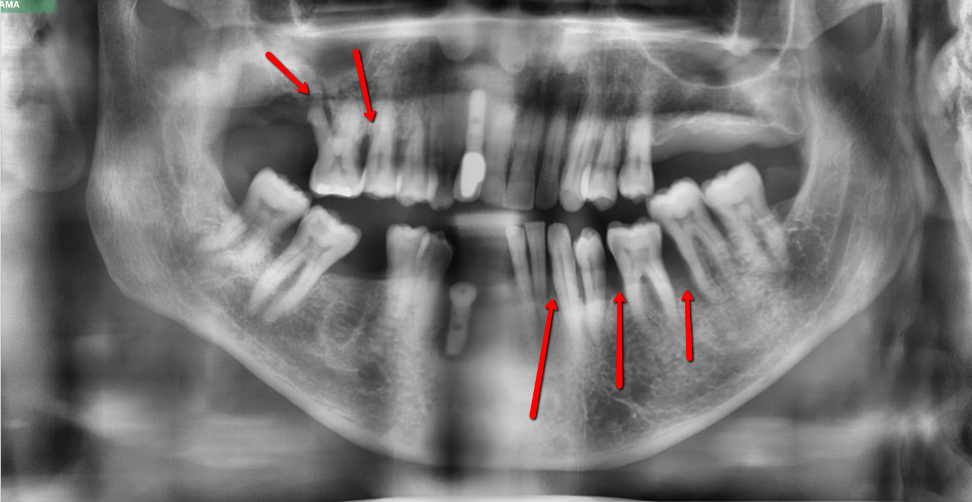
And in these severe cases, unfortunately, sometimes you can’t even treat it with gum surgery. Sometimes unfortunately you may lose the tooth.
Examining your Periodontal Probing Depths
So, we said one way to diagnose whether you have periodontal disease is to look at the x-rays. The other way is also by measuring your gums. So, you’re probably familiar when you go to your dentist’s office and your hygienist or dentists are always measuring your gums with this little periodontal probe here.
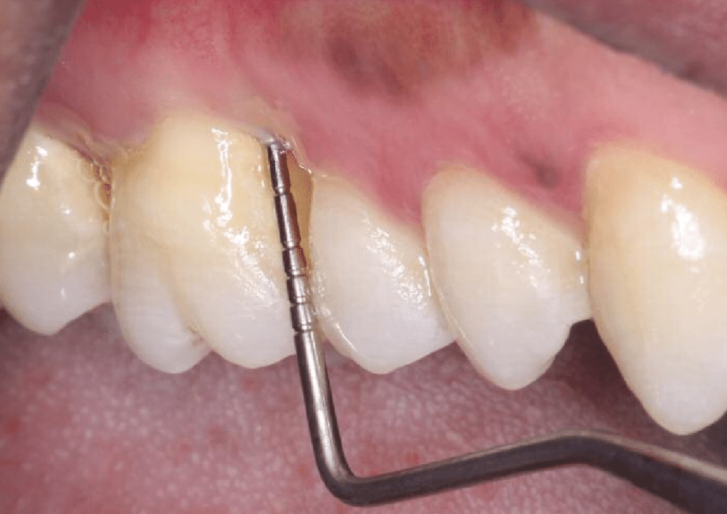
It has little markings on it that basically tell us how much separation your gums have from the root of your tooth. The deeper that your probe can go, the more that means that we have more separation of your gums due to the inflammation. The deeper your probe goes; it tells us the worse your periodontal disease is. We measure your gums to determine how bad your periodontal disease is.
Gingival health
One to three millimeters deep is healthy.
Mild Periodontal Disease
Four millimeters is where you start to be on the cusp of potentially needing a deep cleaning. If you have a lot of four-millimeter pockets throughout your mouth accompanied by bleeding, then you will most likely need a deep cleaning.
Moderate Periodontal Disease
If we do see four to five millimeters with bleeding generalized throughout your mouth, that patient is definitely leaning more towards needing a deep cleaning.
Severe Periodontal Disease
If a patient has six millimeters plus probing depths, they’ll probably start out with a deep cleaning, but honestly, it’s not going to be good enough. That patient will most likely have to go visit a periodontist to look at some periodontal surgery options.
Deep Cleaning versus Osseous Surgery
These treatment options that we are talking about are a deep cleaning versus going and visiting a periodontist to get some sort of periodontal surgery.
Deep Cleaning
In regard to deep cleanings, we typically numb up your mouth and we try to get as deep underneath your gums as possible to remove that bacteria. The problem is that if the bacteria are deep under your gums when we try to get our instruments as deep underneath there as possible, we can only typically get to about five millimeters depth. Any deeper than that then our instruments can’t really see what’s going on down there or reach far enough, so we’re not really able to remove all of your bacteria. If we leave residual bacteria underneath, then the bacteria can multiply and continue to release toxins and therefore not solve the problem.
A common question I receive when I tell a patient they need a deep cleaning or gum surgery is “I don’t understand why this is happening? I brush my teeth and floss like crazy.” The problem is that bacteria not only accumulate up top on top of the tooth, but it develops underneath your root surfaces too. To make things worse, it’s mineralized and hardened and that’s why when you’re brushing and flossing, that it’s not really removing any of this bacterium. Because of the mineralization and hardening underneath your gums, you need to go see a professional such as a dentist or a dental hygienist to get that bacteria removed.
They typically use special tools such as an ultrasonic scaler to go deep underneath your gums to try to scrape away as much of that bacteria as possible. Just remember we can’t go that deep underneath your gums if your periodontal pockets are too deep.
If deep cleaning is not an option for you because your measurements are too deep and you’ve lost too much bone over the years, then you need to look at another option called gum surgery. Its technical name is osseous surgery. And I know once we say surgery, it sounds scary, but I’ll go into a little bit more detail as to why it’s not that bad.
Osseous Surgery
Gum surgery is a loose term. It involves any surgery involving your gums. When it comes to performing gum surgery that’s specifically removing the bacteria underneath your gums, then it is referred to as osseous surgery. What we do is we peel the gums back and clean out all that calcified bacteria on the root surfaces and we also get rid of the diseased bone and then stitch the patient back up. Traditional osseous surgery is more invasive, but it is tried and true. We’ve been doing it for over 60 years. It does tend to have some side effects such as severe root sensitivity and more post-operative pain. In certain cases, we also can regrow bone. However, that can definitely add a lot of cost to your procedure.
Osseous Surgery versus LANAP (Laser) Surgery
LANAP (Laser Gum Surgery)
There is however another option to remove bacteria underneath your gum without cutting your gums. It is called laser gum surgery. This was invented about 15 years ago with a procedure called LANAP. They use a specific wavelength laser to destroy the bacteria that are underneath your gums. It can also regrow bone in certain instances. Overall, it’s a great less invasive option to achieve the same thing of reducing the bacteria underneath your gums.
All right. So, when you compare those two options, obviously LANAP sounds a bit better because osseous surgery is more invasive. In laser gum surgery, we don’t have to peel your gums back. But osseous surgery does have one major benefit in that it’s usually a little bit cheaper if the dentist doesn’t add a lot of bone grafting. That’s a big if. So that is where you have to be careful because a lot of dentists or periodontists are going to add on a lot of expense with bone grafting. I’ll explain a little bit more later where the extra bone grafting might not even make a difference because you might not even need it.
Other benefits of laser gum surgery are it’s less invasive and less painful and it has a quicker recovery time. So, that’s where you get the added benefit of laser gum surgery. It is a bit more expensive than traditional osseous surgery, however, you don’t have to pay for extra bone grafting with laser gum surgery. So in the end, when you visit some of these different dentists, you actually will probably save more money with laser gum surgery.
What You Need To Look Out For!
As I mentioned at the beginning of this post, a lot of times there are dentists and dental hygienists that will tell you that you have gum disease and you need a deep cleaning. As a periodontist in practice since 2011, I’ve gone to a hundred different dental practices in my career as an independent contract surgeon and I’ve met a lot of people. I’ve seen a lot of dental hygienists and I’ve seen how some of these corporations set quotas and standards upon the dental hygienists in regards to what their expectations are for every patient being diagnosed for deep cleaning. Honestly, it’s unethical.
This is the reason I made this blog post. It’s because I want everybody to be educated about the periodontal disease to be able to truly know if they really do need a deep cleaning. I’m not saying that all dental offices are all out to get you to make sure that you pay more money or use all your insurance benefits to get this deep cleaning. I just want to make sure that if you need it, then you actually do need it, and that you are as an informed patient as possible. Also, I want you to know basically all the criteria that you might have within your mouth versus just going into your dentist and blindly accepting the treatment that they offer you.
Some questions you may ask your dentist or hygienist
So, here are some things that you can ask if you get diagnosed with periodontal disease.
Do you have five-millimeter probing or greater?
Do you have a lot of bleeding in your mouth when they probe your gums? You can even ask to have a handheld mirror and be looking at your mouth when they’re probing your gums.
Are your gums very sensitive when they probe? That might be an active sign of inflammation. It’s like touching a bee sting on your arm. The more you touch it, if it’s inflamed, then it would obviously be sensitive.
Also, ask to see your x-rays. Do you see any bone loss?
These are certain things that you can ask that can help you truly know whether you need a deep cleaning or not. However, even these questions will not 100% tell you whether you need a deep cleaning or not. If you have any doubts about this, then you should definitely go and seek a second opinion. Unfortunately, dentistry can be very subjective sometimes, so it definitely could be a benefit to go seek a second opinion.
Now, let’s say that you’ve been told that you need some sort of surgery, whether osseous surgery or LANAP. What are some things to be looking out for? Well, there are some dentists out there that if they tell you that you need that osseous surgery, they may tell you that you have a lot of bone loss and you need to add more bone. Well, if somebody tells you that at the time of your consultation, a lot of times it is extremely difficult to be able to tell whether a patient truly does need bone grafting or not. Most of the time, it is extremely difficult based on your x-rays to determine whether bone grafting will be effective.
There are certain offices or dentists which then start adding what we call bone graft and membrane onto each tooth within the mouth. What that really does is that drives up the overall cost of the procedure and obviously the expense for the patient. Personally in my career, I have seen a lot of patients that come to me for a second opinion that have been diagnosed with that and they get these ridiculous $15,000 to $20,000 treatment plans. It’s very unfortunate because I really feel that it’s an abuse of the system and an abuse of the patient’s trust. If you feel that you get this type of treatment plan, it might be a good idea to go and seek a second opinion and really ask whether you truly need all that extensive bone grafting. I don’t see this all the time, but I have seen it many times in my career.
If you are getting laser gum surgery, what are some things to be aware of in those situations? Well, be wary of dentists who tell you that they can rebuild all the bone with laser gum surgery. I think a lot of patients do a little research online and they say, “Oh. Can LANAP rebuild all the bone that I’ve lost?” And as amazing as LANAP is, and it can give you great results with less invasive procedures, anybody that has a lot of experience with laser gum surgery would be lying to you if they said that they can rebuild all the bone within your jaw bone all the time. I find that it is pretty unpredictable. I find it has to do with the patient’s oral hygiene, the extent of disease, and the current degree of inflammation. There are so many different factors involved in regards to trying to predict whether a patient is going to get bone growth.
Another abuse that I’ve seen with patients is when patients obviously would love to try to save every tooth that they can. But a lot of times we see patients that have such extensive bone loss that the best treatment option for that patient would be extraction and may be looking at an option like an implant or a bridge or an All on Four if enough of their teeth are severely diseased. So whenever a patient is being told that laser gum surgery or osseous surgery is a good option for that patient, sometimes some doctors basically get a little too overzealous when they tell patients they can save the patient’s teeth and how much time that a patient can buy from having this laser gum surgery done. These are some of the other things to be looking out for if you’re going to have laser gum surgery or osseous surgery.
Final Advice
Remember, periodontal disease occurs due to bacteria. Your dentist having to go in to remove that bacteria under your gums is only half the battle. How you take care of your teeth after in regards to extensive tooth brushing, (two to three times a day), using mouth rinses, using floss, using interproximal brushes, will determine how long you will keep your teeth in good condition. I know that sounds like a drag, but if you want to hold onto your teeth and maintain the esthetics of your mouth and not have to undergo something like dental implants or a procedure called all-on-four or having dentures, it’s just well worth the investment.
You need to make sure that you’re dedicated to taking care of your teeth. I like to tell patients that taking care of their teeth is like losing weight. You can go meet a trainer, train with that person for six months who will also help you with your diet. But if you lost all that weight that you wanted to lose or gained all that muscle that you wanted to gain, if you don’t do a good job of taking care of your teeth after your procedure, it’s all for nothing. Just as if you were to not take care of your diet and your exercise afterward, you can just regain all that weight that you had lost with your trainer.
Your periodontist doing your surgery is only fighting half the battle against your periodontal disease. Remember there is no cure for periodontal disease. It is just a situation like hypertension, diabetes, where we try to manage it. Your periodontist will be able to get rid of the bacteria and get you back to health. Just understand, a lot of this is going to be on you also to take care of the results that you get. And if you don’t do a good job with taking care of your teeth and you have old habits that come back and you never floss your teeth again, or you brush your teeth once a day, or you go to the dentist every two years, you’re not going to maintain good results and the bacteria is going to come back and then start re-accumulating underneath your gums. And then you’re going to find yourself in that situation again three, four, or five years down the road.
I hope this information was helpful for you in your fight against periodontal disease. Good luck!

